It’s me and you. One in every two Australians are living with or dying early from chronic diseases. Take a moment to consider what this ‘total burden’ of disease costs – in just one year it’s the equivalent of robbing Australians of 4.8 million years of healthy life. What a devastating waste of humanity!
The Australian Government’s Institute of Health and Welfare (AIHW) releases report after report on Australia’s health, year after year and its latest report, Australian Burden of Disease Study: Impact and causes of illness and death in Australia 2015, for the first time, the total burden from living with illness (50.4%) was greater than the burden from premature death (49.6%).
Non-communicable diseases (NCDs) are the leading cause of illness, disability and death in Australia. Coronary heart disease is the leading cause of premature death, followed by dementia and Alzheimer’s disease, stroke and lung cancer. A third of this disease burden could be prevented by addressing four modifiable risk factors – alcohol consumption, tobacco use, nutrition and physical activity.
Knowledge and evidence is not the problem. The problem is that the Australian Government hasn’t had a preventive health plan for years, despite giving commitments to the United Nations and pledging to act on World Health Organization (WHO) recommendations.
Ending Australia’s preventive health policy vacuum
Australia’s public health sector responded with collective applause when Health Minister Greg Hunt made a cameo video appearance at the Public Health Prevention Conference in Melbourne last Wednesday to announce the development of a new National Preventive Health Strategy.
Was this a genuine signal that the Coalition Government is ready to lift its game on preventive health?
With the election win behind them, the Government seems to be doing a slow U-turn on tackling NCDs, promising a new robust national framework. This would be a critical first step in rectifying former Health Minister Peter Dutton’s damaging decision to shut down Australia’s national preventive health system five years ago.
The result was that most of Australia’s preventive health work came to a standstill because of budget cuts, policy inertia and the dismantling of Labor’s Australian National Preventive Health Agency – despite the evidence that public health interventions are cost-effective and game changing.
Minister Hunt’s announcement means the Prevention 1st campaign, which is led by FARE, the Public Health Association of Australia and the Consumers Health Forum to put ‘preventive health’ on the political agenda, has been accomplished.
Now for the real work.
And there is a lot to do because as the Prevention 1st Scorecard showed when it was published and launched at Parliament last year, Australia is not going well – in truth, we have a disconcerting and disheartening record.
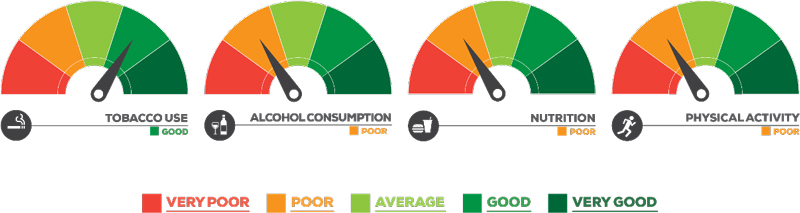
The Scorecard result was ad-hoc progress on the prevention and control of NCDs and inconsistent implementation of policies across the country. A score of ‘good’ was achieved for tobacco, but the record for alcohol, physical activity and nutrition was poor.
This disappointing record is a function of a failure by Australian governments to prioritise prevention which manifests itself in low-level investment in preventive health. The 2017 report Preventive Health: How Much Does Australia Spend and is it Enough? showed Australian spending on health prevention is well below that of comparable countries, such Canada and New Zealand.
The report found Australia spends just over $2 billion on preventive health each year, or around $89 per person. At just 1.34 per cent of Australian healthcare expenditure, the amount is considerably less than OECD countries Canada, New Zealand and the United Kingdom, with Australia ranked 16th out of 31 OECD countries by per capita expenditure.
The need for action is clear, but until Minister Hunt’s words are turned into meaningful action – and spending – NCDs will continue robbing Australians of quality of life while increasing health care costs.
What we need now is a robust process that can quickly and systematically lock-in a strategy and program of action that leans heavily on the WHO’s prescription for action. To do otherwise will mean public health has been conned again – one third of preventable chronic disease will go on and the toll of death and disability will continue as a heavy burden on the health system, taxpayers and Australian families.







